Pretende organizar um evento?
Admeus, tudo o que precisa numa só plataforma!

Admeus, tudo o que precisa numa só plataforma!

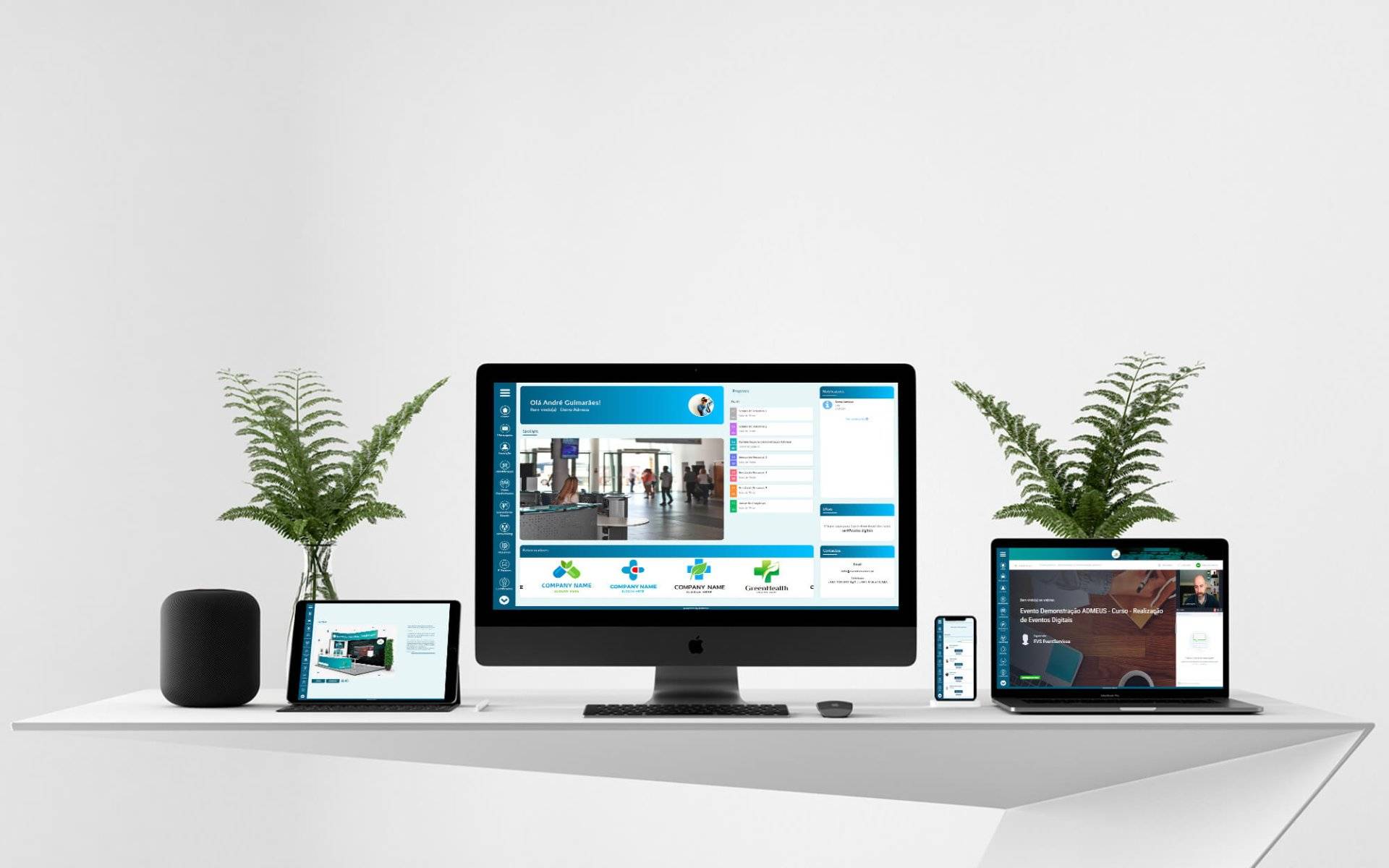
Local e online em plena sintonia. Veja abaixo as nossas soluções.

Apresentadores e participantes reunidos sem necessidade de um local físico.


Visite o nosso site demo de demonstração, registe-se e veja tudo o que o Admeus pode fazer pelo seu evento.

É uma plataforma online especializada na gestão de eventos e tem como objetivo principal facilitar todo o processo envolvente na organização e gestão, antes, durante e após o evento.
A plataforma foi lançada com o intuito de realizar todo o tipo de eventos, desde simples reuniões com poucos participantes a congressos com milhares de pessoas.
Com esta ferramenta o seu evento tem acesso a um website com formulário de inscrições totalmente personalizável, submissão de resumos, pagamentos automáticos, certificados digitais, newsletters e videoconferências (streamings, conferências virtuais, webinars e formações) em qualquer dispositivo e em qualquer lugar.
Para facilitar o acesso de todos os intervenientes de um evento, o Admeus possui várias funcionalidades que respondem às necessidades digitais do mundo actual, tornando-se assim uma ferramenta essencial para um evento de sucesso.


Visite o nosso site de demonstração, registe-se e veja tudo o que o Admeus pode fazer pelo seu evento.
© 2022 Admeus . All Rights Reserved. | Powered by Event Services